Hospitalization Is Never an Effective Treatment for High-risk Suicidal Clients
Treatment associated with reduced psychiatric symptoms and suicidal behavior. Know the Risk Factors for Suicide.

Five Profiles Of Adolescents At Elevated Risk For Suicide Attempts Differences In Mental Health Service Use Journal Of The American Academy Of Child Adolescent Psychiatry
A statement of interest in suicide is a strong warning sign of suicide particularly if a client has a clear plan and the means to enact that plan.

. Initiate a 11 level of observation. Yet the historic roots of mental health management and care has left a certain legacy. They find that suicide risk post-hospitalization is 100 times greater than average immediately following discharge.
I am afraid I might actually do it the 31-year-old woman told me. A new study published on Wednesday tracked suicide risk among nearly 50000 patients hospitalized for self-harm during a 15-year period. Like previous research this study found a major increase in suicide risk in the month and year following a hospitalization indicating the need for better mental health support and a hard look at how hospitals treat mental health.
Document the plan to mitigate the risk for suicide in the EMR. When symptoms dont improve with treatment however hospitalization might be. Most patients in the high risk group do not kill themselves.
Question 2 5 out of 5 points Hospitalization is never an effective treatment for high-risk suicidal clients. Suicide risk is significantly higher in patients who received less than the median duration of hospital treatment. Outpatient providers on the.
The decision to hospitalize patients at imminent risk for suicide requires careful assessment of risk factors including sociodemographic psychiatric general medical and mental status considerations. June 3 2017. Which is never a factor in assessing suicide risk.
Abigail not her real name was referring to ending her own life. Threatening suicide posing a danger to others and being gravely disabled which is often result of a severe active pyschotic decompensation. Of suicide attempters never attend their first appointment or maintain treatment for more.
In 2017 over 47000 Americans age 10 or older died by suicide. Treatment of psychiatric diagnosis does not necessarily result in reduction of suicide risk. The risk for suicide.
Assessment of these risk factors is essential and can usually be accomplished in a straightforward manner although clinical obstacles sometimes make. Beliefs and thoughts often observed in individuals who are suffering from psychotic episodes due to schizophrenia dementia a manic episode or substance intoxication. These treatments are usually effective in treating people with depression.
The need for standardization in suicide risk assessment. DBT aims to provide treatment to high-risk clients in the least restrictive setting possible. Question 3 5 out of 5 points No single instrument can accurately predict suicide risk without significant.
Exam 3 Question 1 5 out of 5 points The possibility that a person thinking about suicide will kill himself or herself is quite low. Suicide over the life cycle. Hospitalization is never an effective treatment for high-risk suicidal clients.
With regard to suicidal risk the authors argue that suicidal patients are by definition seen as mentally ill and out of control which demands hospitalization and the treatment of the mental disorder often using a medication-only approach. I was curious whether my colleagues recoiled at the callers diagnosis her. In 2013 A suicide death every 128 minutes 2nd leading cause of death among 2534 year olds 3rd leading cause of death among 1524 year olds 4th leading cause of death among 1865 year olds 45 of suicide decedents seek contact with a.
Risk factors assessment and. Which is considered the most effective way to allow clients to express their real selves without categories imposed on them by the interviewed. And many studies have shown that suicide risk is particularly high following discharge from psychiatric inpatient or ED settings Appleby et al 1999.
Direct inquiry concerning suicidal ideation in patients with risk factors is associated with more effective treatment and management7 8 because it allows the physician to gain necessary. For years she had struggled with depression and she teetered on the brink of suicide. A new meta-analytic study published open-access in JAMA Psychiatry this week synthesizes over fifty years of research on suicide rates following psychiatric hospitalization.
This study demonstrates that there are 2 sharp peaks of risk for suicide around psychiatric hospitalization one in the first week after admission and another in the first week after discharge. PSYC 317 Crisis Chap. Medication had helped her only minimally.
Hospitalization can be life-saving and helpful but it always causes. Suicide is the second leading cause of death among individuals ages 15 to 34 the third leading cause of death among children in the age range of 1014 years old and the fourth leading cause of death in those aged 35 to 54 1 2Since 1999 the age-adjusted suicide rate in the United States has. Affective disorders have the strongest impact on suicide risk in.
Lithium in bipolar affective disorder no RCT but Baldessarini et al 1999 shows evidence in review of studies RCT in progress Clozapine in schizophrenia one RCT. Current practices in the treatment of patients who presented with suicidal ideation or. Inpatient carewhich offers medically supervised programs in a hospital setting 24 hours a day 7 days a week and typically ranges from 48 hours to 10 daysis designed to mitigate immediate risk begin treatment and prepare patients for continuing care after hospitalization.
However she never acted on them and was not suicidal currently. Most people who commit suicide are in high risk group and a few are from the low risk group. Notify the ED Practitioner of both the risk for.
Unfortunately the tools to assess risk do not really help determine which patient is going to commit suicide unless precautions are taken. So the rate of false-positive prediction is high11 Second the risk. This kind of routine monitoring is critical to enable therapists to intervene when suicide urges are high as well as to assess the factors that lead to increases and decreases in suicidal urges over time.
TRUE or FALSE. Reduce the use of psychiatric hospitalization. 2 Background Suicide is a frequent cause of death Over 41000 deaths in the US.
If the patient is found to be at moderate or high risk for suicide the RN in the ED will.

Major Depressive Disorder And Treatment Resistant Depression Targeting Suicidal Ideation Psychiatry Advisor

Nimh Advancing Training In Suicide Prevention Clinical Care Day 1
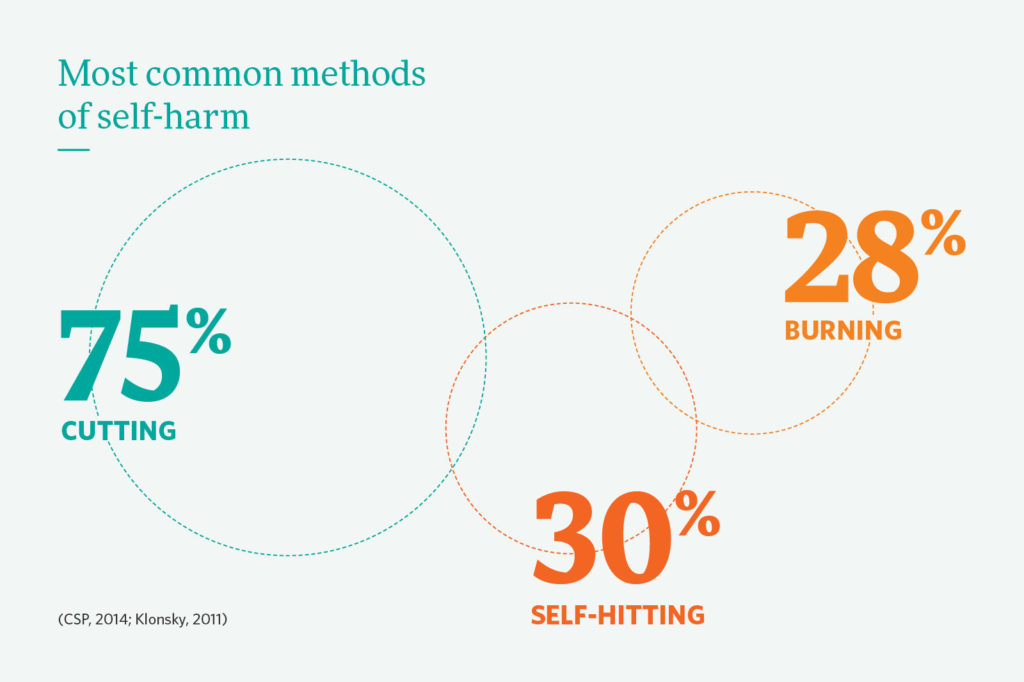
Suicide Prevention In Pediatric Populations

Suicide Prevention In Pediatric Populations

Collaborative Assessment Management Of Suicidality Cams About

Suicide Suicidal Signs Behavior Risk Factors How To Talk More
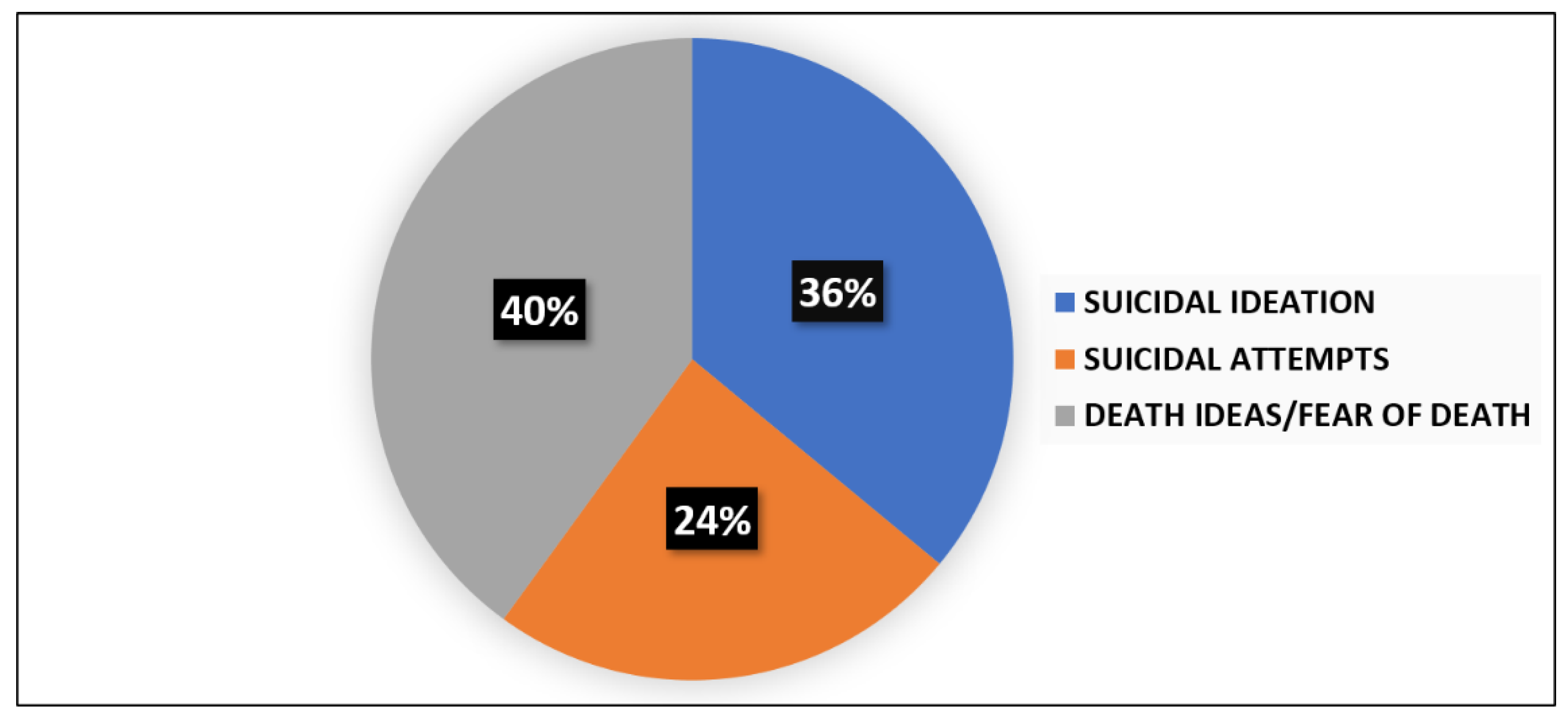
Brain Sciences Free Full Text Suicidal Behavior And Club Drugs In Young Adults Html
Evaluation Of An Emergency Department Educational Campaign For Recognition Of Suicidal Patients The Western Journal Of Emergency Medicine

Evidence Based Suicide Screening And Prevention Protocol For Licensed Nursing Staff A Systematic Literature Review And Recommendations Journal Of Psychosocial Nursing And Mental Health Services

Suicide Prevention In Pediatric Populations

Suicide Suicidal Signs Behavior Risk Factors How To Talk More

Suicide Prevention In Pediatric Populations

Suicidal Behavior Among Elderly Inpatients Prbm

Five Profiles Of Adolescents At Elevated Risk For Suicide Attempts Differences In Mental Health Service Use Journal Of The American Academy Of Child Adolescent Psychiatry

Is The Pandemic Fueling A Rise In Suicide Attempts Among Kids Shots Health News Npr

Comments
Post a Comment